Out of the many acne treatment options available, Ayurvedic and home remedies make use of sandalwood. Sandalwood is an evergreen medium-sized tree, which has mature bark with a pleasant fragrance. Like turmeric powder, this is also used in most of the beauty or skin care products. In oily skin, dirt Continue Reading
Out of the many acne treatment options available, Ayurvedic and home remedies make use of sandalwood. Sandalwood is an evergreen medium-sized tree, which has mature bark with a pleasant fragrance. Like turmeric powder, this is also used in most of the beauty or skin care pro ... Continue Reading
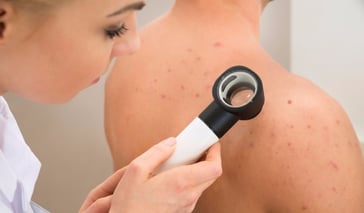
Acne can be an unsightly, but a harmless problem. Acne is due to a problem in the pilosebaceous unit, which is found all over the body, with some exceptions such as the soles of the feet, palms and a few others. There are a few ways to cure acne, which usually involve antibiotic medication or natura ... Continue Reading
Acne can be an unsightly, but a harmless problem. Acne is due to a problem in the pilosebaceous unit, which is found all over the body, with some exceptions such as the soles of the feet, palms and a few others. There are a few ways to cure acne, which usually involve antibi ... Continue Reading
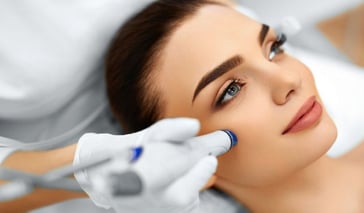
Microdermabrasion can be used for acne scars, as well as to reduce or erase fine lines and wrinkles, giving you a more beautiful, radiant and youthful appearance. Microdermabrasion has made it possible for some people to reduce the visibility or even erase the acne scars, but there of course will be Continue Reading
Microdermabrasion can be used for acne scars, as well as to reduce or erase fine lines and wrinkles, giving you a more beautiful, radiant and youthful appearance. Microdermabrasion has made it possible for some people to reduce the visibility or even erase the acne scars, bu ... Continue Reading
If you are suffering from acne and the over the counter ointments and stinging pads have not worked to cure your acne, you should try one of the best and most proven methods of getting rid of acne safely and naturally. Using basil tea for acne treatment has been around for centuries and is used not ... Continue Reading
If you are suffering from acne and the over the counter ointments and stinging pads have not worked to cure your acne, you should try one of the best and most proven methods of getting rid of acne safely and naturally. Using basil tea for acne treatment has been around for c ... Continue Reading
There are numerous acne treatment options available today. Some people try the instant relief way with peels, while others prefer herbal and home remedies. Turmeric is a spice belonging to the ginger family, and it has been used since olden days as an effective antiseptic. Turmeric can also be used ... Continue Reading
There are numerous acne treatment options available today. Some people try the instant relief way with peels, while others prefer herbal and home remedies. Turmeric is a spice belonging to the ginger family, and it has been used since olden days as an effective antiseptic. T ... Continue Reading
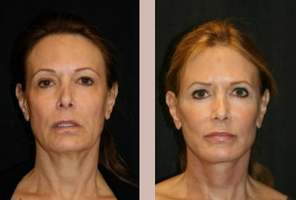
Some types of acne scars cannot be comprehensively cured using conventional acne treatment methods. This is commonly observed in acne scars with deep pits, such as boxcar scars. These acne scars are characterized by a deep abase, wherein the surrounding scar tissue hardens into thick layers that don ... Continue Reading
Some types of acne scars cannot be comprehensively cured using conventional acne treatment methods. This is commonly observed in acne scars with deep pits, such as boxcar scars. These acne scars are characterized by a deep abase, wherein the surrounding scar tissue hardens i ... Continue Reading
Like many medicinal herbs, calendula flowers are also used for acne treatment. When you experience a hormonal change or when excess oil is generated, the pores on the skin get clogged with dirt. Such clogged pores are a breeding place for bacteria, as they can multiply rapidly here. Bacterial infect ... Continue Reading
Like many medicinal herbs, calendula flowers are also used for acne treatment. When you experience a hormonal change or when excess oil is generated, the pores on the skin get clogged with dirt. Such clogged pores are a breeding place for bacteria, as they can multiply rapid ... Continue Reading
Everyone has unique skin, which is why there are so many different types of acne treatment solutions on the market and in the home remedy sections of books. If you haven’t tried using the healing, curing and preventing effects of strawberries before, now is the time. For many people, these homemad ... Continue Reading
Everyone has unique skin, which is why there are so many different types of acne treatment solutions on the market and in the home remedy sections of books. If you haven’t tried using the healing, curing and preventing effects of strawberries before, now is the time. For m ... Continue Reading
Acne treatment may be topical or may be made up of oral medications or solutions that will act from the inside out to clear the skin. Haemafine syrup is a treatment that will act as a blood purifier, resulting ultimately in clearer skin and diminished acne symptoms. Ingredients of Haemafine Syrup Ha ... Continue Reading
Acne treatment may be topical or may be made up of oral medications or solutions that will act from the inside out to clear the skin. Haemafine syrup is a treatment that will act as a blood purifier, resulting ultimately in clearer skin and diminished acne symptoms. Ingredie ... Continue Reading
Nobody wants to have acne scars. It is normal for teens, however, to face acne problems due to hormonal imbalances worsened by pollution and dirt in the environment. Hormonal imbalances naturally occur as a person grows. Pimples disappear, but scars usually remain, leaving marks and blemishes on the Continue Reading
Nobody wants to have acne scars. It is normal for teens, however, to face acne problems due to hormonal imbalances worsened by pollution and dirt in the environment. Hormonal imbalances naturally occur as a person grows. Pimples disappear, but scars usually remain, leaving m ... Continue Reading